The Modern Guide to Immune Health: Diet, Lifestyle, and Environment
The immune system is not a single entity but a complex, balanced condition. It is a biological defense strategy conserved through evolution to resist infection, illness, and undesirable biological invasions while maintaining tolerance to prevent allergies and autoimmune disorders. However, modern life—characterized by specific dietary habits, environmental toxins, disrupted sleep schedules, and stress—can significantly weaken these defenses. Below is a detailed exploration of how these factors influence our immunity.
1. The Impact of Diet and Nutrition
The Western Diet vs. Traditional Diets
One of the most significant factors influencing immunity is the shift toward a “Western diet,” characterized by high intakes of saturated fats, sugar, and salt, and low intakes of fiber. A study comparing healthy men from Tanzania revealed that switching from a traditional African diet (rich in whole grains, fiber, and fermented foods) to a Western diet for just two weeks triggered inflammation and reduced the immune system’s ability to respond to pathogens. Conversely, traditional diets appear to support healthy metabolic and immune processes.
Macronutrients and Inflammation
• Fats: Not all fats are equal. Saturated fatty acids can directly trigger inflammation by interacting with Toll-like receptors (TLR4) on immune cells, confusing the body into thinking it is under bacterial attack. This can lead to “leaky gut,” allowing harmful substances into the bloodstream. Omega-6 fatty acids, found in many cooking oils, may contribute to inflammation if consumed in excess. In contrast, Omega-3 fatty acids (found in fish) are anti-inflammatory. They interact with transcription factors to down-regulate pro-inflammatory genes and produce mediators called resolvins and protectins that clear inflammation.
• Sugars: Simple, processed sugars can reduce the ability of white blood cells to perform phagocytosis (engulfing harmful particles) and may increase inflammatory markers in the blood.
• Salt: High salt intake has been linked to increased inflammation mediated by IL-17, potentially worsening autoimmune diseases.
The Role of Micronutrients Malnutrition and micronutrient deficiencies severely compromise immune cell trafficking and response. Specific vitamins and minerals are critical:
• Vitamin A: Essential for the growth and differentiation of immune cells (T-cells) and maintaining mucosal barriers.
• Vitamins C and E: These antioxidants improve the activity of natural killer cells and lymphocyte proliferation while reducing damage from free radicals. Smokers, in particular, require extra antioxidants to combat the toxicity of tobacco.
• Vitamin D: Regulates both innate and adaptive immunity; deficiency is common and detrimental.
• Trace Elements: Zinc deficiency reduces immune function, while supplementation can boost cytokine production. Selenium and Copper are also vital for the bacteria-killing ability of neutrophils.
Obesity and Eating Disorders
Obesity leads to a state of chronic, low-grade inflammation. Adipocytes (fat cells) release inflammatory cytokines like IL-6 and Tumor Necrosis Factor (TNF). High levels of leptin in obese individuals can overstimulate the immune system, eventually leading to a “resistance” where the immune system becomes less responsive to actual infections. Conversely, eating disorders like anorexia and bulimia reduce the number and function of white blood cells and complement proteins due to calorie and nutrient deficiencies.
Gluten and Genetically Modified Foods (GMOs)
In some animal models, gluten has been shown to stimulate inflammation via TLR4 pathways, distinct from the specific autoimmune reaction seen in Celiac disease. Regarding GMOs, concerns exist that pesticide-resistance genes in crops could potentially be transferred to gut bacteria, or that pesticide residues (like glyphosate) could induce cellular toxicity, though data on human health impacts remains under investigation.
2. Gut Health and the Hygiene Hypothesis
The Microbiome
The gut flora acts like a “sparring partner” for the immune system, providing essential training. A mother’s diet and microbiome can shape her offspring’s immunity, seeding the fetus with bacteria even before birth. Dysbiosis (imbalance of gut bacteria), caused by high sugar and fat intake, disrupts this education, leading to poor immune tolerance.
The Hygiene Hypothesis and “Old Friends”
The “Hygiene Hypothesis” is often misunderstood as a recommendation to be less clean. In reality, it is better described as the “Old Friends” hypothesis. It suggests that the modern lack of exposure to specific ancient microbes (such as helminths and environmental bacteria) that co-evolved with humans has led to a rise in allergies and autoimmune diseases. These “old friends” are necessary to tune the immune system and regulate the balance between TH1 (defense) and TH2 (allergic) immune responses. Public health hygiene (clean water, sanitation) remains vital for stopping deadly crowd infections like cholera, but the loss of contact with diverse environmental microbes has consequences for immune regulation.
3. Lifestyle: Stress, Sleep, and Circadian Rhythms
The Immunology of Stress Stress triggers the Hypothalamic-Pituitary-Adrenal (HPA) axis and the Sympathetic Nervous System, releasing cortisol and catecholamines.
• Acute Stress: Short-term stress (fight-or-flight) can temporarily enhance immunity by mobilizing immune cells (NK cells and neutrophils) into the blood to prepare for potential injury.
• Chronic Stress: Long-term stress is detrimental. It keeps cortisol levels elevated, which eventually suppresses the immune system, reduces T-cell proliferation, and impairs the antibody response to vaccinations. Paradoxically, chronic stress can also increase pro-inflammatory cytokines, raising the risk of heart disease and autoimmune flare-ups.
The Circadian Clock Almost every cell in the body, including immune cells, operates on a 24-hour circadian rhythm regulated by the suprachiasmatic nucleus in the brain.
• Immune Timing: Leukocyte numbers fluctuate daily; neutrophils peak during the day, while lymphocytes peak at night. Disrupting this rhythm (e.g., shift work, jet lag) is linked to heightened inflammation and increased cancer risk.
• Blue Light: The biological clock is synchronized by light, specifically blue wavelengths detected by melanopsin receptors in the eye. While blue light during the day boosts alertness, exposure to artificial blue light (screens, LEDs) at night suppresses melatonin—a hormone crucial for immune regulation and sleep. Chronic misalignment of this rhythm is associated with diabetes, obesity, and depression.
Sleep Sleep is when the body repairs and regenerates. Lack of sleep impairs the ability to fight viruses and increases the risk of illness.
4. Environmental Toxins and Habits
Alcohol and Smoking
• Alcohol: Excessive consumption suppresses the immune system, making it harder to combat viruses and diseases. Experts recommend limiting intake to one drink per day for women and two for men.
• Smoking: Tobacco smoke is highly toxic, damaging lungs and requiring the body to use up its antioxidant stores to combat the damage.
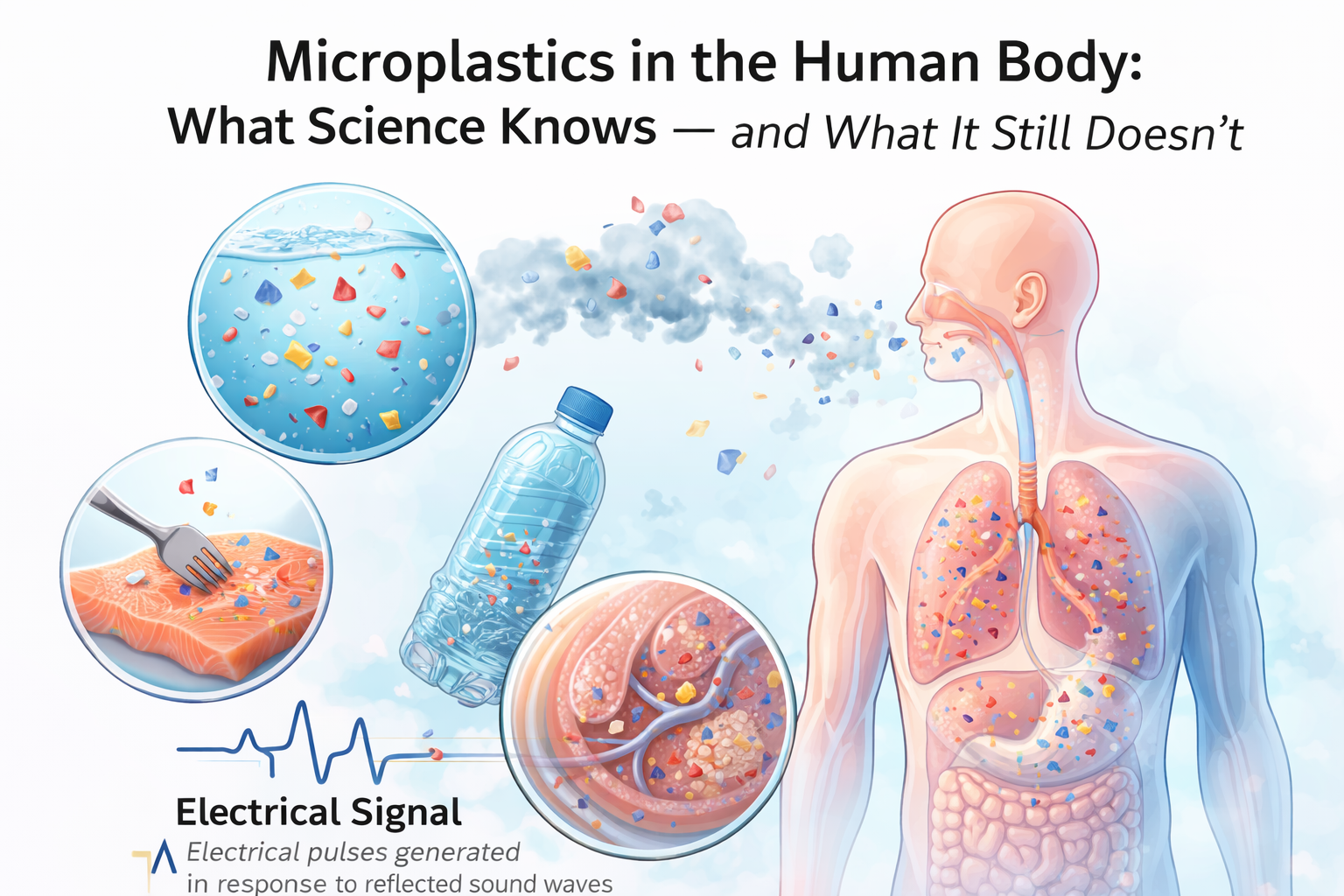
Microplastics (MPs) We are exposed to microplastics through ingestion (food and water), inhalation, and skin contact.
• Internalization: MPs can be taken up by cells through endocytosis. Once inside, they can disrupt signaling pathways, damage mitochondria, and cause oxidative stress.
• The “Trojan Horse” Effect: MPs in the environment develop a “protein corona” or adsorb heavy metals and organic pollutants on their surface. When ingested, they act as vectors, carrying these toxins and even pathogens (like bacteria or viruses) deep into the body.
• Immune Reaction: The immune system recognizes MPs as foreign. Neutrophils may attack them by releasing extracellular traps (NETs), but massive uptake can cause immune cell death and chronic inflammation. MPs have been detected in human blood and feces, indicating widespread systemic exposure.
Multi-Generational Toxin Effects Research indicates that environmental toxins affect more than just the exposed individual. A study on dioxins (industrial by-products) found that maternal exposure weakened the immune response (specifically T-cell function) not only in the offspring but in subsequent generations, up to the great-grandchildren. This suggests that our immune resilience is partly determined by the environmental exposures of our ancestors.
Building a resilient immune system requires a multi-faceted approach. It involves adopting a nutrient-dense diet rich in fiber and antioxidants, maintaining a diverse microbiome, managing chronic stress, synchronizing our lifestyle with natural circadian rhythms, and minimizing exposure to environmental pollutants like plastics and smoke.
Also Read: